Hysteroscopy is a surgical procedure in which a long thin camera, or scope, is inserted into the uterus to evaluate the uterine cavity for causes of abnormal bleeding. Hysteroscopy can be performed in the office or in the operating room. It can be diagnostic (just to look and identify the problem) or operative (to look, identify, and remove the problem)1.

An office hysteroscopy is conveniently performed in a physician’s office under local anesthesia. Numbing medication is injected into the cervix and a very thin camera is guided into the uterine cavity.
An office hysteroscopy can identify abnormalities involving the uterine cavity:
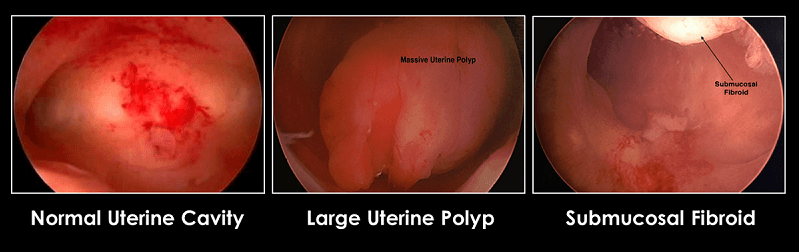
A small biopsy can be performed during the evaluation to rule out malignancy. If fibroids or intrauterine adhesions are found, operative hysteroscopy under IV sedation in the operating room will be required.
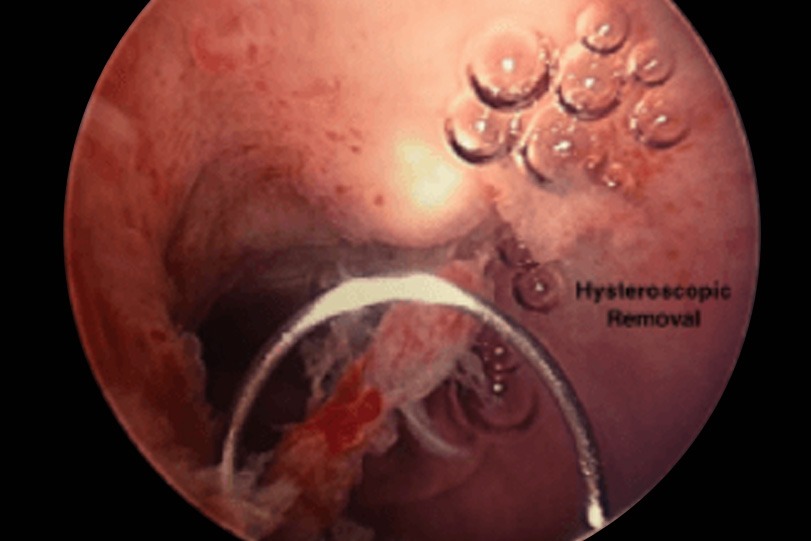
Operative hysteroscopy removes intrauterine growth (fibroid or polyp), uterine septum, or adhesions. This procedure is performed in the operating room under IV sedation administered by an anesthesiologist.
During the procedure, the cervical canal is dilated and a larger-caliber camera (scope) is guided into the uterine cavity. The uterine cavity is distended with fluid and a heated loop device is then used to cut away the fibroid (hysteroscopic myomectomy), polyp, septum, or adhesions. In cases of large fibroids, uterine septum, or extensive adhesions, several procedures are required for complete removal and should be performed by an experienced surgeon to avoid complications.
One of the risks of operative hysteroscopy is the formation of intrauterine adhesions. In some cases, an intrauterine balloon is placed at the completion of the procedure to decrease bleeding and prevent scarring. The balloon is removed in the office after seven days, and the patient is prescribed high-dose estrogen for several weeks to rebuild a healthy uterine lining and further prevent the formation of intrauterine adhesions.
Back to TopWhile recovering from a hysteroscopy:
Some of the risks and complications associated with a hysteroscopy include:
At The Center for Innovative GYN Care® (CIGC®), we believe doing extensive research before choosing a surgeon is important. Get to know our surgical specialists and see why they are the best in the industry.
When performing any procedure at CIGC, our goals are to:
We have performed thousands of laparoscopic procedures for all types of GYN conditions, including fibroids, endometriosis, pelvic masses, pelvic pain, and GYN cancers. We are renowned both nationally and internationally for our results.
Women choose CIGC because GYN surgery is the only medicine we practice. We have made a commitment to performing hysteroscopy and other gynecological procedures, and our specialists are board-certified and fellowship-trained in minimally invasive surgery. We do not use open or robotic procedures, so we can achieve our goals of treating your condition with as little pain as possible.
Our laparoscopic procedures are top-of-the-line, providing the smallest number and size of incisions possible. Rather than having a long, expensive procedure and painful recovery, you will be back on your feet in no time.
Our specialists are ready to provide an evaluation of your symptoms and conditions and recommend an appropriate solution.
Back to Top1 Centini G, Troia L, Lazzeri L, et al. Modern operative hysteroscopy. Minerva Ginecol. 2016 Apr;68(2):126-32
Back to TopSchedule a consultation to learn more about how we can treat your condition today.