1. Laparoscopic-Assisted Myomectomy Surgery with Bilateral Uterine Artery Occlusion/Ligation
Published in The Journal of Minimally Invasive Gynecology MacKoul P, Danilyants N, Baxi R, van der Does L, Haworth L.
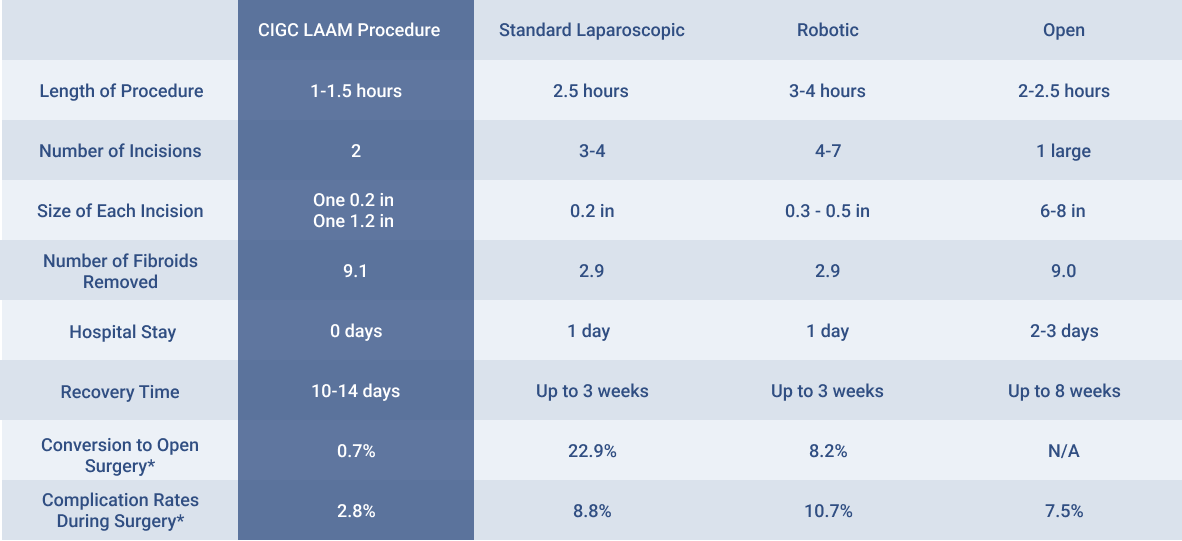
In the comparison of 1,313 patients who underwent a myomectomy (the review included patients who had LAAM®, robotic, standard laparoscopic, or open myomectomy surgery), LAAM (laparoscopic assisted abdominal myomectomy) showed the best patient outcomes, including removal of large and multiple fibroids, lowest complication rates, and the lowest conversion to open surgery at 0.7 percent. Patients interested in fertility had temporary occlusion of the uterine arteries thereby maintaining full blood flow to the uterus.
2. LAAM: Surgery Center Versus Outpatient Hospital
Published in The Journal of Obstetrics and Gynecological Research (JOGR), March 2020. Natalya Danilyants, Mamta Mamik, Paul MacKoul, Louise vanderDoes, Leah Haworth
A comparison of the LAAM procedure performed in the hospital vs the surgery center revealed the same results, with the no differences in the number and weightof fibroids removed, patient weight or prior surgery, or any other factors.
3. LAAM at a freestanding ambulatory surgery center: A case series
Published in Gynecolgical Surgery, June 2020. Paul MacKoul, Natalya Danilyants, Faraj Touchon, Louise vanderDoes, Leah Haworth, Nilofar Kazi.
LAAM performed in 969 women in the ambulatory surgery center can be performed safely in the freestanding ambulatory surgery center even in women who are morbidly obese.