The treatment of abnormal bleeding is directly related to the cause. Abnormal bleeding can be heavy, irregular, or sporadic. Once a diagnosis is made, targeted surgical or medical therapy is then used to treat the problem. Sampling of the uterine lining is necessary in most cases, can help with the diagnosis, can be performed in the office with endometrial biopsy or more comfortably in a surgery center setting with better control and less pain.

A Hysteroscope is used to look inside the uterine cavity for a biopsy
Patients with abnormal bleeding must seek a diagnosis and treatment immediately. Benign conditions such as fibroids, adenomyosis, and endometriosis will progress with time, causing increasing pain, fertility, and resulting anemia. Fertility can be severely affected by all three of these conditions if they are not managed rapidly and appropriately. Watching and waiting is not an option. If your OBGYN is not providing a diagnosis and treatment plan, seek a second opinion with a CIGC surgeon for more information and treatment options.
Premenopausal and postmenopausal patients with abnormal bleeding are at higher risk for uterine and cervical cancer. Endometrial biopsy, or better hysteroscopy with biopsy must be performed to rule out malignancy. Watching and waiting is never acceptable for patients with pre and postmenopausal bleeding, and consultation with a CIGC surgeon is recommended for appropriate and immediate care.
Back to TopThere are many causes of abnormal bleeding, most of which are from the uterus. Severe bleeding is a cause for concern since a more serious condition may be present. Anemia can result causing weakness and even syncopal episodes (fainting), which can be dangerous. Patients with abnormal bleeding need to be diagnosed and managed quickly.
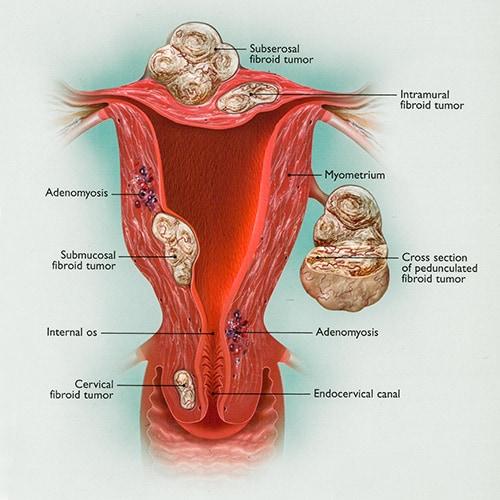
Common causes include Fibroids, Adenomyosis, Endometriosis, Uterine, and Cervical Polyps (overgrowths).
Less common causes include endometrial hyperplasia (overgrowth of the uterine lining causing bleeding), uterine cancer, and cervical cancer.
For a more detailed discussion of each condition, please go to the Conditions section or to Treatment Options for more information.
Finally, there are some medications that will cause bleeding, such as birth control methods, blood thinners, and others. Medical conditions such as hormonal imbalances from the ovaries, the pituitary and thyroid glands (hypothyroid), and many more can result in abnormal uterine bleeding.
Dysfunctional uterine bleeding (DUB) is uterine bleeding that has no known cause and is a common diagnosis made in those patients without any of the factors above.
Back to TopMost common causes and treatments for abnormal bleeding that are approved by CIGC are listed below.
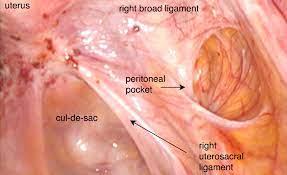
Endometriosis involving the base of the uterus, the pelvis (culdesac), and the peritoneum of the right uterine sidewall.
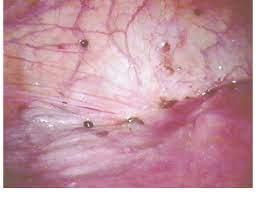
Endometriosis of the peritoneal lining – black and brown implants of disease.
3. Adenomyosis – the lining of the uterus growing into the muscle. Dualport GYN hysterectomy is the only reasonable long-term option. Medical therapy can be used for those who desire fertility, but the effects are not long-term.
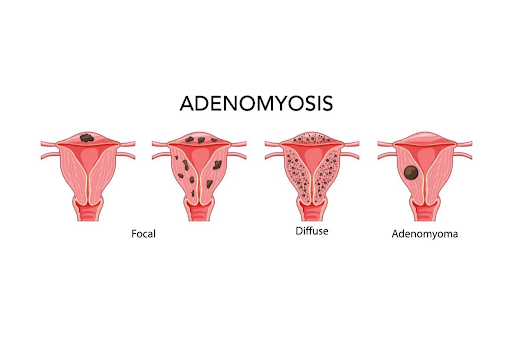
Focal adenomyosis is localized to the muscle, whereas diffuse disease is throughout the uterus. An adenomyoma is a collection of adenomyosis. For more information refer to Adenomyosis in the Conditions section.
4. ENDOMETRIAL HYPERPLASIA – overgrowth of the uterine lining that is not malignant or atypical can be treated with hormone therapy if fertility is desired. For those with atypical hyperplasia, which has a 30 – 40% chance of cancer present, a Dualport GYN hysterectomy is the best option.
5. UTERINE OR CERVICAL POLYPS – removal of the polyps. These are rarely malignant.
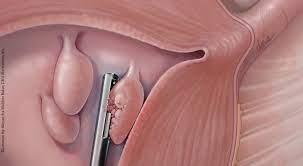
Uterine polyps being removed with hysteroscopy
6. UTERINE CANCER – Dualport GYN hysterectomy, removal of ovaries, and staging to include lymph node evaluation.
7. CERVICAL CANCER – Dualport GYN hysterectomy and staging.
8. DYSFUNCTIONAL UTERINE BLEEDING – DUB – is treated with hormone therapy, or ablation, which is the destruction of the lining of the uterus. Ablation of the uterine lining, either by thermally (heating) the lining or burning, has limited utility. The procedure is effective for those with dysfunctional uterine bleeding. Ablation works if the lining is normal, is not involved with fibroids, and the uterus does not have adenomyosis. Unfortunately, many patients are subjected to this procedure with both, and the results are disappointing. For cases that are not completely managed by these options, a Dualport GYN hysterectomy is required.
Back to TopLAAM myomectomy and Dualport Hysterectomy provide exceptional outcomes with smaller incisions, faster recovery, less pain, lower complications, and much lower cost to the patient than robotic, standard laparoscopic, or open procedures. These procedures are performed in a surgery center setting, greatly increasing patient satisfaction while decreasing infection, COVID transmission, and costs.
Back to TopSchedule a consultation to learn more about how we can treat your condition today.