ENDOMETRIOSIS EXCISION
By Paul MacKoul, MD - Laparoscopic GYN Surgeon and Co-Founder of CIGC
Advanced Laparoscopic Techniques for Endometriosis Excision
Endometriosis excision refers to the removal of endometriotic implants while preserving the uterus, tubes, and ovaries. While endometriosis has no cure, proper and complete laparoscopic excision, followed by appropriate medical management, allows for better pain control and the preservation of fertility. Medical management is the use of birth control pills, and other hormonal therapy to slow down the progression of disease. Medical management should not be used in place of a surgical procedure to diagnose, remove, and treat endometriosis — but should be used after all of the disease has been surgically excised. No physician should ever dismiss severe and progressive pain with menstrual cycles as normal or just “bad periods.” If your OBGYN or another physician is not responding to your needs, seek out a specialist for help.
Endometriosis is the most common cause of pain and infertility in patients of reproductive age. Endometriosis is generally a small-volume disease, meaning that the implants of endometriosis are so small they cannot be detected by ultrasound, CT scan, or MRI. It is classified according to the location, depth, and spread of the disease. Laparoscopic surgery is the first and most important step in both diagnosis and treatment of endometriosis — it allows for early detection and removal of the disease. Unfortunately, this disease is often not detected early, with many patients being improperly managed by their OBGYN, leading to a misdiagnosis or a delay in treatment. A delay in treatment, and no diagnosis of this disease, leads to persistent and worsening pain, extensive scarring, infertility, and eventually chronic pelvic pain1. Patients with pelvic pain should always be ruled out for endometriosis first, before other sources of pain, such as bladder and bowel, are considered. The use of continuous birth control pills or other management schemes should not be the first option for care.
Implants of endometriosis are small areas of the disease in which the lining of the uterus (the endometrial lining) is outside and growing on the ovaries, tubes, bladder, bowel, and other pelvic structures. The best treatment for implants of endometriosis is surgical resection, or complete removal. OBGYNs often burn or cauterize the implants, leading to incomplete destruction and increasing scarring and pain.
Patients with a suspected diagnosis of endometriosis should always see a endometriosis specialist, such as the physicians at The Center for Innovative GYN Care® (CIGC®). Specialists are fellowship-trained to identify and excise all disease safely and effectively. Laparoscopic specialists devote their entire practice to surgery, and do not perform obstetrics. CIGC surgeons are specialists providing superior overall care for patients with endometriosis, which results in better pain control and fertility management.
Surgical Techniques
Surgery is the first and best management for the diagnosis, excision, and treatment of endometriosis. Implant excision is the removal of small areas of disease involving any surface or organ system2. Excision to areas such as the bladder, bowel, ureters, and large vessels, as well as to the ovaries and tubes, should always be performed by a fellowship-trained laparoscopic surgeon for the best results. Many OBGYNs are not trained in excising endometriosis to these structures, and the vast majority of patients treated by OBGYNs with endometriosis to the bladder, bowel, and ureters do not have the disease excised at the time of surgery. Excision should always be used, not cauterization. Cauterization is often called burning or fulguration of the implants. After surgical excision, medical therapy can be used to better control, but not prevent, the progression of endometriosis.
Surgical Excision of Endometriosis
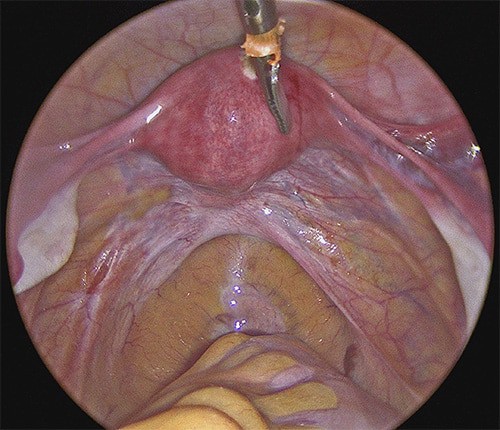
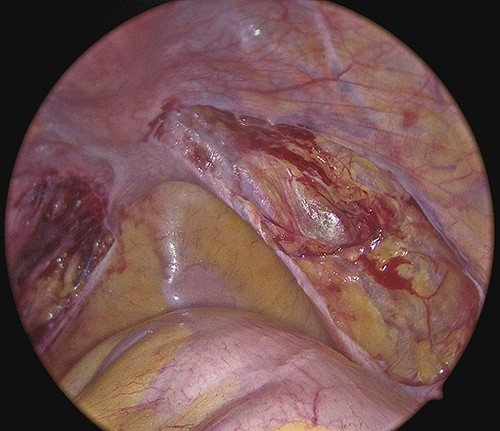
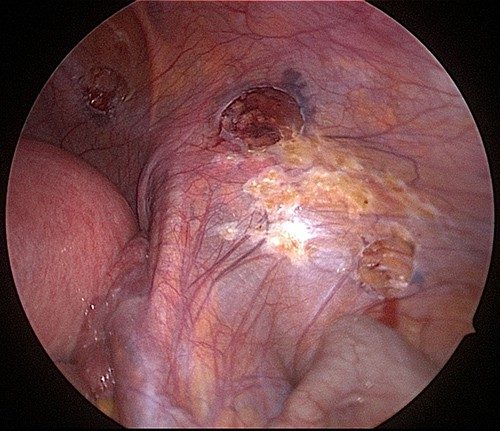
Cauterization of Endometriosis vs Excision
Endometriomas are large collections of endometriosis involving the ovaries. These cystic collections of disease should never be drained, which is a common OBGYN method of treatment. Drainage leads to recurrence of the disease faster, with close to 90 percent of patients having recurrence, as well as further spread3. Excision of the lining of the endometrioma is required to fully remove all disease but must also avoid removal of the surrounding ovarian tissue. Unfortunately, many patients undergo needless removal of a complete ovary, or removal of a large amount of surrounding ovarian tissue when endometriomas are surgically removed. Only in rare situations in which the entire ovary is replaced by endometriosis should the ovary be removed. We use our powerful DualPortGYN® technique for this procedure to minimize recovery time, complications, and pain.
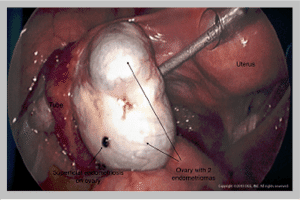
The CIGC Difference
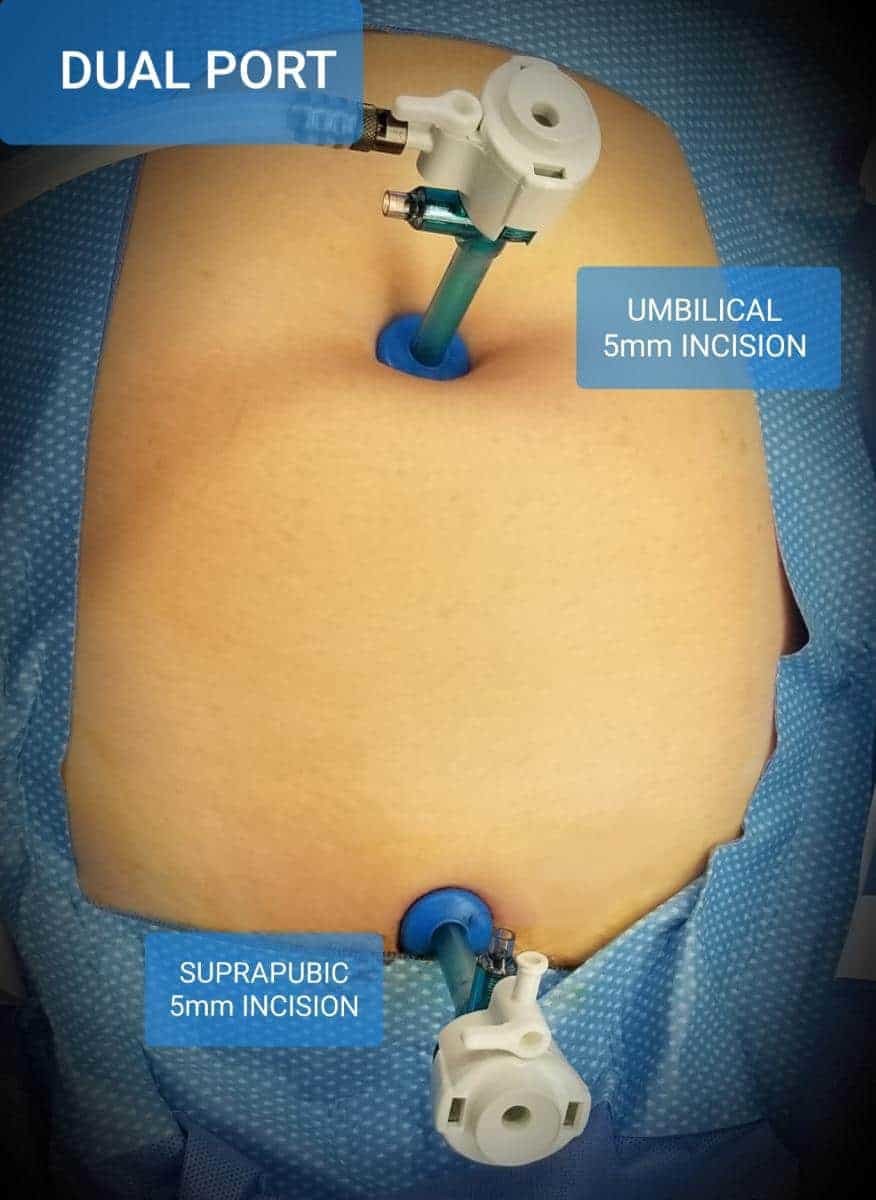
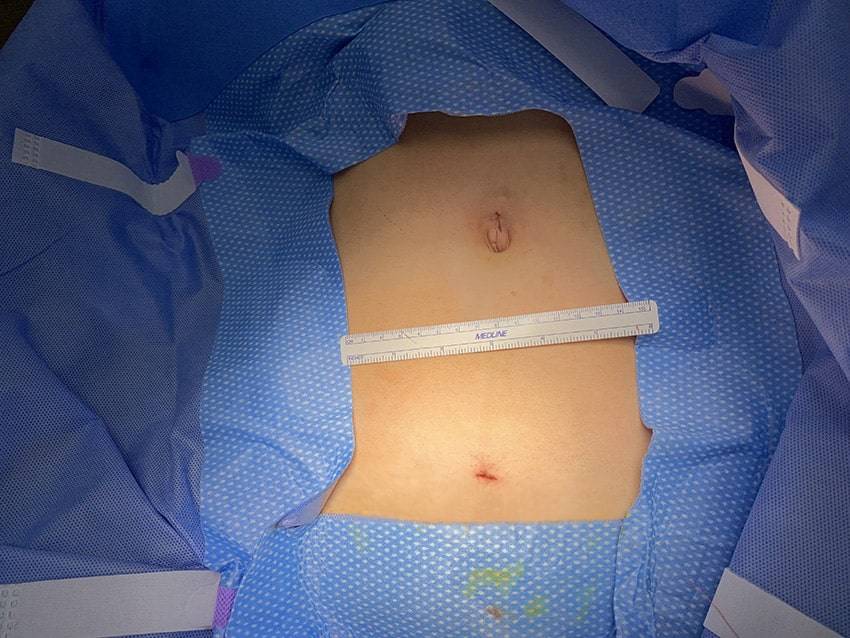
CIGC surgeons often use DualPortGYN retroperitoneal techniques to excise even the most extensive implants or cystic collections (endometriomas) quickly, safely, and effectively. Retroperitoneal techniques allow for the full evaluation of the pelvis, and by identifying vital structures such as the bladder, bowel, ureters, and large vessels, success rates are very high, and complication rates are very low. DualPortGYN often uses only two to three 5 mm — ¼ inch — incisions for the complete resection of all disease. Compared to robotic approaches using four to five incisions with the overall length of the incisions being up to five times the length, DualPortGYN results in fewer and smaller incisions, a safer procedure, and faster recovery time.
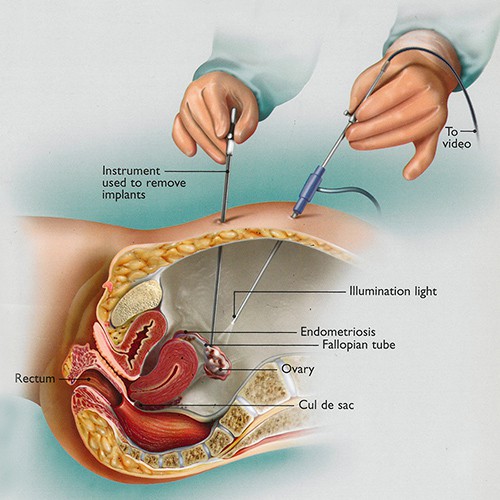
During endometriosis excision surgery, a thin telescope-like camera is inserted into the navel to evaluate the pelvis. Usually, one to two additional 5 mm skin incisions in the lower abdomen are made to access the pelvis, and the endometriotic implants can be dissected out and removed. For severe endometriosis with extensive adhesions, it is sometimes not possible to completely resect all of the endometriosis, as it may be deeply involved with vital structures such as the ureter or rectum. Women interested in maintaining fertility undergo surgical excision of the disease. Many of these women may become pregnant after surgical excision, but a significant number will require in vitro fertilization (IVF) to allow for pregnancy due to the inflammatory effects of endometriosis on fertilization and implantation. For women who are done with childbearing or who have not responded to conservative management, a hysterectomy may be recommended for longer-term relief.
All patients undergoing excision of endometriosis, from those with minimal disease to those with extensive disease or requiring a hysterectomy, will go home the same day as surgery. Recovery times usually range between three to five days, with up to seven to 10 days required for more extensive surgery. In all cases, patients are able to walk the first day and are mobilizing easily on the second day.
Prior to your surgery:
- All patients need to complete preoperative testing within 14 days of the surgical date
- Fax all preoperative testing results to your surgeon’s office at least five days prior to surgery, unless instructed otherwise
- A nurse will contact you one to two days before your scheduled day of surgery to review your medical history and preoperative instructions
- You cannot have anything to eat after midnight the night before the procedure
- Do not take any aspirin products or blood thinners one week prior to your surgery
- Bathe or shower with Hibiclens soap (found at the drugstore) the day of or the night before the surgery
- Wear loose fitting clothing, and no jewelry or make-up or creams/lotions on your skin
- Please bring your insurance card and picture ID and any form of copay
- The surgery scheduling team will send to your local pharmacy the appropriate prescriptions for after surgery
- All patients must have an adult escort to take them home due to anesthesia; you may not go home in a taxi unaccompanied
- If you have any preoperative or postoperative questions, please contact your surgeon’s office
Endometriosis Excision Surgery Recovery
What to Expect After Endometriosis Excision Surgery
In the process of recovering from endometriosis excision surgery, these possible side effects may occur:
- Pain
- General pain: Pain should resolve over time and will get better every day
- If pain persists or becomes worse, a visit to the ER is recommended
- Pain around the incision sites is not uncommon and will resolve over several days. Most patients describe pain as minimal or moderate and improving daily.
- Chest and shoulder pain: The carbon dioxide gas used to insufflate the abdomen during the procedure (so the surgeon can see) will sometimes irritate the phrenic nerve, which leads to mild to severe pain. This nerve tracks pain impulses from the lining of the chest cavity. The pain can occur during deep breaths. This resolves within two to three days and is not worrisome. If the pain is extreme or does not resolve, a visit to the local ER is important to rule out other causes of chest pain.
- General pain: Pain should resolve over time and will get better every day
- Bleeding
- Vaginal spotting is common for the first week and should then resolve on its own. Call the office if you have heavy bleeding, increased bleeding, a foul odor, or if you have urinary or rectal bleeding.
- Nausea
- Anesthesia is the main cause for nausea immediately after surgery. After the first 24 hours, nausea is more likely caused by either your narcotic pain medication or antibiotics. If you are experiencing severe nausea, please call your doctor.
- Swelling
- Swelling of extremities: Swelling of the legs and sometimes arms is not uncommon after surgery. This is due to increased fluid given during the procedure. This will resolve over several days. If you notice persistent or increasing swelling, tenderness to the calf, or calf pain, please call the office immediately.
- Abdominal swelling: Some degree of distension (swelling) is to be expected after surgery. This is due to irritation of the intestines and resolves over time. It is usually mild to moderate only.
- Constipation
- Constipation can cause pain that can get worse with increased amounts of medication. If you experience constipation, drink lots of fluids and eat a high fiber diet. You may also use a mild laxative, such as Milk of Magnesia, or a stool softener, such as Colace. No prescription is required for either.
- Diarrhea
- Diarrhea is sometimes caused by antibiotics and will resolve once the antibiotics are stopped. A probiotic such as lactobacillus can help with this process. Rarely, severe diarrhea can develop. Call your doctor if you have severe diarrhea, bloody diarrhea, or if your diarrhea is accompanied by fever or worsening pain.
- Urinary retention
- Urinary retention is the inability to pass urine through the bladder. A very small number of patients will develop this problem due to the anesthetic used for the surgery. Most patients will have their bladder catheter removed immediately after the surgery. If you are sent home and are not able to pass urine, please go to a local ER. A catheter will be placed to allow the bladder to rest after the surgery and will be removed no less than five days after the surgery. It is important to have this catheter placed to avoid injury to the bladder.
- Bruises/Scars
- Some patients will develop bruises at the incision sites. The incision sites are made by trocars, plastic sleeves used for access during the surgery for the camera and for instruments. Sometimes these trocars cut tiny vessels just beneath the skin that cause limited bleeding. Even under the best of circumstances, it is sometimes impossible to see these small vessels. A bruise will develop that will resolve on its own. Those patients with very large masses or fibroids may also develop bleeding at the incisions that can be more extensive due to longer manipulation of the trocar sites. Rarely, this bleeding can be very extensive, leading to a large bruise that tracts to the groin area. Please note that this type of bleeding almost always resolves. Pain or warmth may develop from the blood under the skin. Use Motrin 600 mg every six hours or 800 mg every eight hours to relieve the pain.
Endometriosis Excision Surgery Recovery Time
- Getting back to work
- Return to work after endometriosis excision surgery is dependent on each individual patient. If you are feeling well and want to return to work, please do so. If you have any questions, call your doctor for advice.
- Sex
- Intercourse should be avoided for at least two weeks. Once you are feeling comfortable, then you may resume intercourse.
- Driving after surgery
- Driving can begin only after you have stopped taking narcotics, and if you feel strong enough to be able to stop the vehicle in an emergency. If you are not confident, have someone drive you.
Endometriosis Excision Surgery Recovery Tips
- You will be given a prescription for Motrin prior to surgery and a narcotic at the facility prior to your discharge
- To be effective, Motrin should be used in doses of 600 mg every six hours, or 800 mg every eight hours. Narcotics should be used sparingly since they will cause constipation. The first several days following surgery, most patients use mainly Motrin or extra-strength Tylenol during the day, along with a narcotic sometimes at night to help with sleep. Using a heating pad on the lower abdomen is safe. Coughing can be uncomfortable initially because of abdominal discomfort. Placing a pillow on the abdomen for support while coughing can be helpful.
- Use caution when starting an exercise routine after endometriosis excision surgery — start out slowly and gradually work up to your normal time, distance, and speed
Endometriosis Excision Risks and Complications
Additional risks and complications after endometriosis excision include:
- Internal bleeding
- Hernia (rare with small incisions)
- Infection (rare)
- Damage to a blood vessel
- Damage to organs such as the stomach, bowels, or bladder
Endometriosis Excision FAQs
Ready for a Consultation
If you’re considering endometriosis excision, our specialists are ready to provide an evaluation of your symptoms and conditions and recommend an appropriate solution.
Additional Resources
This PDF presentation provides information on the connection between endometriosis and fertility.
Related Blog Posts
References
1 Agarwal SK, Chapron C, Giudice L, et al. Clinical diagnosis of endometriosis: a call to action. Am J Obstet Gynecol. 2019 Apr;220(4):354.e1-354.e12
2 Singh SS, Suen MW. Surgery for endometriosis: beyond medical therapies. Fertil Steril. 2017 Mar;107(3):549-54
3 Chan LY, So WW, Lao TT. Rapid recurrence of endometrioma after transvaginal ultrasound-guided aspiration. Eur J Obstet Gynecol Reprod Biol. 2003 Aug 15;109(2):196-8
4 Taylor HS, Giudice LC, Lessey BA, et al. Treatment of endometriosis-associated pain with elagolix, an oral GnRH antagonist. N Engl J Med. 2017 Jul 6;377(1):28-40







